 When you find out you are expecting a child, your thoughts immediately turn to expectations. What will the baby be? A boy? A girl? Will the baby look like you or me? Take after my side of the family or yours? Have my curls and your red hair? Have my gutsy laugh and green eyes and your smile and good sense of humor? Will our baby grow up to be a teacher? An artist? A politician? A Nobel Prize winning scientist? The possibilities were as infinite as the limits of the love I felt for this being that we created but had never met.
When you find out you are expecting a child, your thoughts immediately turn to expectations. What will the baby be? A boy? A girl? Will the baby look like you or me? Take after my side of the family or yours? Have my curls and your red hair? Have my gutsy laugh and green eyes and your smile and good sense of humor? Will our baby grow up to be a teacher? An artist? A politician? A Nobel Prize winning scientist? The possibilities were as infinite as the limits of the love I felt for this being that we created but had never met.
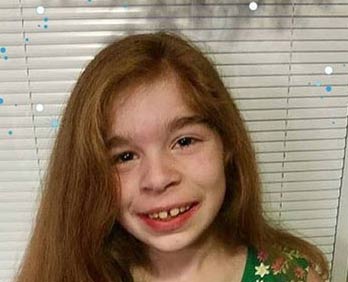
One day in September 2007, we embarked on the journey of finding answers to all of those questions when our daughter, Brenna, was born weighing 6 lbs 15 oz at 5:17 AM on a beautiful day at the Jersey Shore. By the OBGYN’s account she was born 10 days early but I knew she arrived right on time. She had the most adorable pudgy cheeks but was very difficult to feed. Several hours after birth she didn’t seem to prefer formula or breastmilk, slept A LOT and ate VERY LITTLE! I just felt like something wasn’t right. She had hypoglycemia (low blood sugar) after birth and had some tremors but was misdiagnosed with having an immature neurological system. She was admitted to the NICU where they collected samples that were sent off as part of her newborn screening and she spent 3 days in the NICU on a dextrose drip and regular bottle feedings. After her blood sugar levels stayed above 65 they weaned her off the drip, told me to feed her every 2-3 hours and sent her home with me. I asked if I should get a glucometer and monitor her blood sugar but the neonatologists responded to me like I was a hysterical, first time mom. “No, take your healthy baby home and enjoy her.” they said.
The first six months were as anyone would expect … sleep deprived yet blissful. Yet there was one small problem. She was very difficult to feed. It would take hours for her to consume just a few ounces of formula and when she did eat, she’d spit up most of what she drank. So, after repeated trips to the pediatrician where they assured me that she was healthy, growing and developing normally, they told me to change to a more sensitive formula. They, too, told me to “take home your healthy baby and enjoy her.” Not left with a lot of choices, we tried many brands and varieties of formula in an effort to find one that she would not spit up as much and as frequently, to no avail.
Six months after she was born, in March 2008, she had a seizure right in front of me. It was the first one I’d seen and recognized immediately as a seizure. God only knows how many she had that were unrecognized or not seen. Words cannot express how incredibly scary and devastating it was to witness that! After talking her through the seizure, she was alert and responsive. So, I picked her up and woke my husband to tell him what just happened. He called the pediatrician to seek his advice. While he was on the phone, I wanted to see if she would take a bottle. I fixed a full 8oz bottle, sat in the recliner and fed her. She drank the entire 8oz bottle in less than 15 minutes, without fussing or spitting up. The pediatrician said he wanted to see her. So, we packed up and drove to his office. When we got there I told him the one thing that seemed off to me was how she consumed a full bottle for the first time in six months in a short amount of time without crying or spitting up most of it. He told us to take her to a children’s hospital of our choice.
We stayed with Brenna for two weeks at a children’s hospital in New Jersey but the doctors there couldn’t figure out what was wrong with her. Over the first week, I kept in constant contact with the pediatrician and told him everything the specialists were telling us. It was our pediatrician who first said the word hyperinsulinism (HI) to me. He explained that he had consulted with some colleagues and poured over my maternity records and her medical records from the hospital, spoke to them about Brenna’s condition, did some of his own research and thought she might have it. He admitted that he had never personally treated a patient with hyperinsulinism in his 30 years of practicing medicine but he was sure that was what she had. To our knowledge her newborn screening had come back normal with nothing to report. However, much to our dismay, it did not include a screening for congenital hyperinsulinism. So, he urged me to research this condition in the computer library for families in the hospital.
After reading some of the information my family and I found on the internet, I begged to be transferred to the Children’s Hospital of Philadelphia (CHOP) After days of waiting for an available bed and transportation we were on our way to Philadelphia. Upon admission, the CHOP HI team was explaining how they were planning to investigate what was happening to our little girl. A few hours later, they checked her vital signs and her blood sugar. To our surprise there was no need to wait, it was already low enough for them to administer a Glucagon injection and find out if Brenna had what they suspected, congenital hyperinsulinism. Moments later, their suspicion was confirmed. Once we received a diagnosis, reality set in and I did what any mother would do. I began the inquisition. The barrage of questions must have seemed limitless like the wonder I felt when I first learned I would finally become a mother. The expectations that I dreamt of when I first learned I was pregnant were quickly replaced by a litany of other questions and a torrent of emotions and that spilled out of my mouth and tear ducts in an emotional rage like a scene worthy of Shirley MacLaine in Terms of Endearment or Sally Field in Steel Magnolias. Why did this happen? What did I do to cause this? Why didn’t they catch this before she was born? Why didn’t the neonatologists and pediatrician screen for it or catch it when she was born? Would she live or die? Would she grow up healthy and act like a normal or average child and live a happy childhood? Would she be able to walk? Talk? Play sports? Would she go to school? Would she be able to drive a car? Would she graduate from college? Would she be able to get a job and become a productive member of society? Would she ever get married? Would she be able to run a marathon? Would she be able to have a baby of her own?
You name it, I asked it and they were only able to answer some of the questions with certainty. The rest we would have to wait and see. Then the flood gates opened. I expressed myself in true gut wrenching fashion that would have made Shirley and Sally proud. I spilled forth every emotion fathomable from the relief and gratitude that we had an answer and a plan, anger that she was not properly diagnosed at birth, when taken to the NICU or released to go home, heartbreak that she would live with this condition for the rest of her life, fear of the unknown impact of her condition caused by six months of chronic hypoglycemia and the stigma of that she would later face as the unknown developmental consequences and the side effects of the necessary lifesaving drug took effect, worry about the life long effect of this medicine on her other organs and whether she’d ever be able to have a child of her own someday, regret for failing as her advocate and not following my first instinct to test her blood sugar after discharge from the NICU anyway, frustration over not being able to get her pediatrician to listen when I repeatedly expressed my concern about her eating habits or lack thereof, and the deepest sorrow that she may not ever be the discoverer of world peace or the cure for cancer grief that the healthy baby I was told to take home and enjoy was in fact not healthy.
The doctors and nurses stood there, silent, patient, listening to every word, consoling me and some crying along with me. We stayed another two weeks while Dr. Charles Stanley and his hyperinsulinism team determined that Brenna had what is known as diffuse HI. They started her on an oral suspension called diazoxide. After a few days they conducted a safety fast to see if the dose of this medication along with eating solids and drinking formula would keep her blood sugar stable. The fast was a failure. She did not fast as long as they wanted. Then, it was determined that the diazoxide, coupled with her food intake, was not enough to sustain her blood sugar at safe levels. So, they added Octreotide and later added diuril due to the fluid retention caused by the high dose of Diazoxide, a drug that she would need for rest of her life. The staff at CHOP told us about their partnership with the University of Pennsylvania and explained they could offer her a diagnostic tool, a PET scan.
We met their world renowned expert surgeons who could determine if her HI could be cured by removing part of or her entire pancreas rendering her a diabetic. We opted to take a conservative approach as she was stable and responding well to the medicine and they agreed and asked us to participate in their research study. They were collecting DNA samples and sending them off for genetic testing that would hopefully lead to an explanation. We gladly agreed to participate in the hopes that we would be able to cure Brenna of this disease. My pregnancy was uncomplicated with no Gestational Diabetes. However, I did have pre-eclampsia and thus was induced. I had a normal, drug-free, vaginal delivery and there is no family history of hyperinsulinism in our families. So, we hoped that this test would unlock the mystery of how we got here. Unfortunately, after weeks of waiting, the genetic test yielded inconclusive results. We had no idea what part of her DNA was affected, whether she could pass this on to her own children or if we would have more children with the same condition. Since she continued to respond so well to the prescribed medications, they were confident that she was well enough to go home. In April 2008, Brenna was discharged from CHOP with prescriptions for diazoxide, diuril, octreotide and an emergency glucagon kit. We were also educated on how to check and monitor her blood glucose at home and given her first of many glucometers and test strips.
Three months after discharge from CHOP we had to stop the Octreotide when she had an episode of dangerously high blood sugar. Doctors at CHOP recommended that we eliminate the Octreotide from her regime because her appetite had somewhat improved with her curious palate that began to enjoy a variety of solid foods more than formula. In the spring of 2009 we started to become anxious and suspicious about Brenna’s developmental milestones. Brenna was a late walker and talker and still can take or leave eating (unless it was something she REALLY loves such as M&M’s, hot dogs, chicken nuggets…typical childlike fare). We had her assessed by speech, occupational and physical therapists and they confirmed one of our worst fears. She had significant delays in all three areas but they were confident that with their help, she could regain and overcome these deficits. So, we enrolled her in early intervention services with our local school district where she has undergone years of Speech, Occupational and Physical Therapy to combat the challenges of her developmental delays which she may live with for the rest of her life. To this day, I still relive the emotional roller coaster when our HI journey first began but in spite of all this, we are grateful. While Brenna has overcome much so much in the past few years, she still has significant cognitive and developmental delays.
Through it all she remains positive. She is funny, loving and sees the beauty and the best in everything and everyone. Sometimes, I get off the roller coaster long enough to observe our feisty little girl who is growing up and making strides and then I feel them. The infinite possibilities, and I immerse myself in the wonder. What will she become when she grows up? The answer is simple…anything she wants. While we don’t have all the answers we know one thing for certain she will always be her Mommy’s baby and her Daddy’s girl, just like we dreamed she would be.

